Ringworm is a common fungal skin infection that spreads easily and often looks like a thin red circle on the skin. Despite the name, there are no worms involved. The condition comes from dermatophyte fungi that live on skin, hair, and nails, and it can pass between people, animals, and shared items. While ringworm is usually mild, untreated infections can linger and spread to new body sites or household members. The good news is that most skin infections respond well to over-the-counter antifungal creams and simple hygiene steps. However, scalp, nail, or widespread infections need prescription care. Understanding how ringworm starts, how it travels, and how to treat it at home helps you clear it sooner and avoid passing it on.
What Is Ringworm and How Does it Spread?
Ringworm, also called tinea, is a superficial fungal infection that feeds on keratin in the outer layers of skin, hair, and nails. The most common culprits are species of Trichophyton, Microsporum, and Epidermophyton. These fungi thrive in warm and moist environments and can live on skin surfaces and objects like towels and combs. People catch ringworm through close skin contact, by touching contaminated items, or through contact with infected animals. Pets can be silent carriers, so fur loss in a cat or dog warrants attention. Because the infection stays on the surface, healthy immune systems usually contain it, yet spread within households is frequent without treatment and cleaning.
On the body, it favors exposed or sweaty areas. On the feet, it can show up between the toes after hours in tight shoes. On the scalp, it spreads in schools and sports. Understanding these pathways helps you cut transmission while you treat the rash. Incubation usually spans a few days to two weeks. People remain contagious until treatment has begun for 48 hours. Fungal spores may survive on surfaces for weeks, especially in humid rooms. Crowded housing and shared sports gear increase the spread. Consistent cleaning and early treatment reduce household outbreaks. Remind children not to share hats.
How Ringworm Looks on Different Parts of the Body

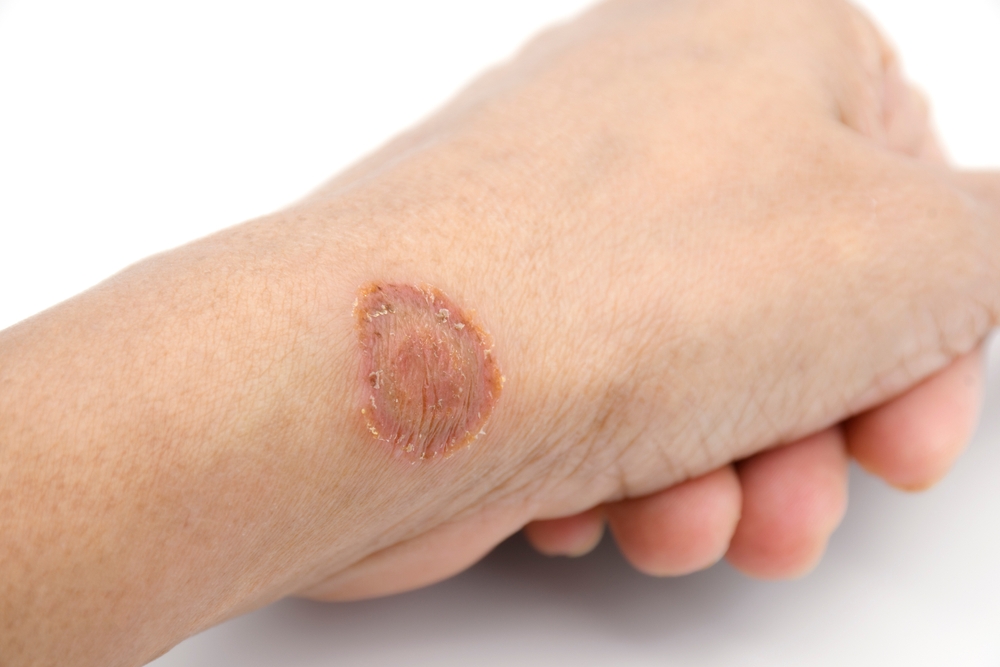
Body ringworm often starts as a small scaly patch that slowly expands outward, leaving clearer skin in the center and a more active border at the edge. Edges can look slightly raised or scaly, and the patch can itch or sting. On darker skin tones, the border may look brown or gray, while on lighter skin it may look pink or red. The face, trunk, and limbs can be involved, and the pattern can be less circular in some cases. Scalp ringworm in children may cause flaky patches, tenderness, or hair loss in irregular shapes. Beard area infection can cause swelling or crusting with hairs that break easily. Foot infections can crack the skin and lead to itching and soreness between the toes.
Nails can become thick and brittle if the infection reaches the nail unit. Doctors confirm uncertain cases by scraping a little scale from the edge and examining it under a microscope or sending it for culture. Groin involvement causes itchy, red scaling along the inner thighs and folds. On the scalp, tiny black dot hairs can mark broken follicles. A tender boggy swelling called a kerion needs prompt care to prevent scarring. Some Microsporum infections fluoresce green with a Wood lamp, though many do not. Facial involvement may lack rings and mimic eczema.
When to Treat Yourself or be Treated by a Clinician
Uncomplicated body or foot ringworm usually responds to non-prescription antifungal creams, gels, or sprays. Many people can start with an over-the-counter imidazole or terbinafine product and expect improvement within a couple of weeks. However, you should seek medical care if the rash is on the scalp, in the beard area, or in the nails because those sites need prescription therapy. You should also get care if the area is extensive, unusually painful, oozing, or not improving after two to three weeks of correct use. People with diabetes, poor circulation, or weakened immunity should involve a clinician early.
Infants and young children who develop scalp patches need prompt evaluation to prevent scarring or long-term hair loss. A doctor can decide whether to use oral medicines, check for bacterial infection, or look for mimics like eczema or psoriasis. Clear guidance on location, size, and response helps you avoid delays. Also seek care if lesions involve the face or genitals, because scarring risk and diagnostic overlap are higher. Recurrent infections deserve a check for athlete’s foot or nail sources. Pregnant people should confirm product safety before starting treatment. Athletes in contact sports need clearance to prevent team spread. Pharmacists can advise on product choice and correct application steps.
Simple At-Home Treatment

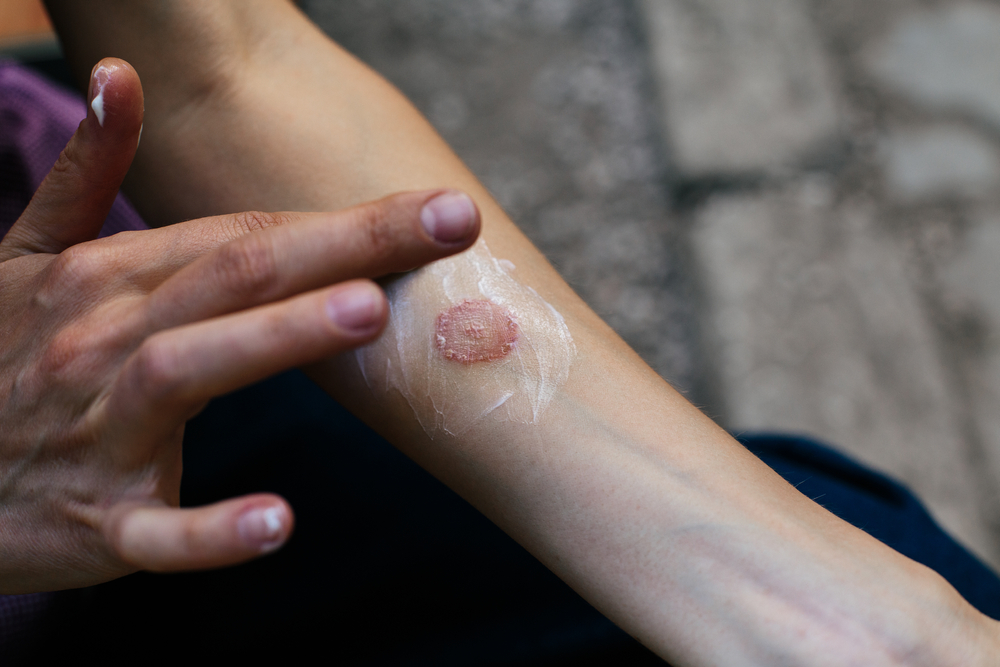
Clean the skin gently and dry it well before applying medicine. Apply a thin layer of the antifungal a little beyond the visible border, because fungi extend into nearby normal-looking skin. Most labels advise treatment once or twice daily. Keep going for the full course and continue for one to two weeks after the rash looks clear, so that microscopic fungi do not remain. Change into dry clothes after workouts and switch out damp socks or underwear once they feel moist. Wash your hands after touching the rash and avoid sharing towels, hats, combs, or razors while treating. Shower sandals help in shared spaces.
Do not use topical steroids for an itchy circular rash without medical advice because they can mask and spread the infection. If itching remains bothersome, cool compresses and loose cotton clothing help with comfort while the antifungal works. These steps shorten the course and cut down on the spread. Trim nails short to reduce scratching and contamination between sites. Use a separate towel for the affected area and launder it hot. Let the shoes dry completely and consider using antifungal powder inside. Choose breathable fabrics that wick sweat and reduce moisture. Clean grooming tools after each use to avoid re-seeding skin. Treat athlete’s foot at the same time to prevent reinfection.







0 comments:
Post a Comment